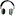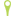Also known as Procedure for Prolapse & Hemorrhoids (PPH), Stapled Hemorrhoidectomy, and Circumferential Mucosectomy
PPH is a technique developed in the early 90's that reduces the prolapse of hemorrhoidal tissue by excising a band of the prolapsed anal mucosa membrane with the use of a circular stapling device. In PPH, the prolapsed tissue is pulled into a device that allows the excess tissue to be removed while the remaining hemorrhoidal tissue is stapled. This restores the hemorrhoidal tissue back to its original anatomical position.
The introduction of the Circular Anal Dilator causes the reduction of the prolapse of the anal skin and parts of the anal mucous membrane. After removing the obturator, the prolapsed mucous membrane falls into the lumen of the dilator.
The Purse-String Suture Anoscope is then introduced through the dilator.
This anoscope will push the mucous prolapse back against the rectal wall along a 270° circumference, while the mucous membrane that protrudes through the anoscope window can be easily contained in a suture that includes only the mucous membrane. By rotating the anoscope, it will be possible to complete a purse-string suture around the entire anal circumference.
The Hemorrhoidal Circular Stapler is opened to its maximum position. Its head is introduced and positioned proximal to the purse-string, which is
then tied with a closing knot.
The ends of the suture are knotted externally. Then the entire casing of the stapling device is introduced into the anal canal. During the introduction, it is advisable to partially tighten the stapler.
With moderate traction on the purse-string, a simple maneuver draws the prolapsed mucous membrane into the casing of the circular stapling device. The instrument is then tightened and fired to staple the prolapse. Keeping the stapling device in the closed position for approximately 30 seconds before firing and approximately 20 seconds after firing acts as a tamponade, which may help promote hemostasis.
Firing the stapler releases a double staggered row of titanium staples through the tissue. A circular knife excises the redundant tissue. A circumferential column of mucosa is removed from the upper anal canal. Finally, the staple line is examined using the anoscope. If bleeding from the staple line occurs, additional absorbable sutures may be placed.
What are the Benefits of PPH over other Surgical Procedures?
1) Patients experience less pain as compared to conventional techniques.
2) Patients experience a quicker return to normal activities compared to those treated with conventional techniques.
3) Mean inpatient stay was lower compared to patients treated with conventional techniques.
What are the Risks of PPH?
Although rare, there are risks that accompany PPH:
4) If too much muscle tissue is drawn into the device, it can result in damage to the rectal wall.
5) The internal muscles of the sphincter may stretch, resulting in short-term or long-term dysfunction.
6) As with other surgical treatments for haemorrhoids, cases of pelvic sepsis have been reported following stapled haemorrhoidectomy.
7) PPH may be unsuccessful in patients with large confluent hemorrhoids. Gaining access to the anal canal can be difficult and the tissue may by too bulky to be incorporated into the housing of the stapling device.
8) Persistent pain and fecal urgency after stapled hemorrhoidectomy, although rare, has been reported.
9) Stapling of hemorrhoids is associated with a higher risk of recurrence and prolapse than conventional hemorrhoid removal surgery; according to a Canadian study of 537 participants.





Readmore...
Friday, January 30, 2009
Stapled Hemorrhoidopexy (PPH Procedure)
Friday, January 16, 2009
Microtia
Microtia: A Common Birth Defect
Every year one of every seven to eight thousand children is born with a common birth defect referred to as "Microtia." Not a life-threatening condition, microtia typically occurs in one ear, but can affect both ears.
While many children born with microtia are normal in all other respects, some have other health conditions including defects of the face and head. Microtia can be, but is not always, a hereditary condition.
Often a mother exposes the fetus to foreign substances without knowing they may harm the developing fetus. Accutane, a drug prescribed to relieve acne for example, if taken in the early weeks of pregnancy may result in microtia or other birth defects. There are likely other toxins doctors do not know of that may result in microtia.
http://www.microtia.com/_fileCabinet/GRBT108-2245G-30-297-312.pdf
Usually the ear forms during the early weeks of the first trimester, when the fetus is most at risk for birth defects. Sometimes doctors do not know the cause or causes for microtia. For some, the causes for microtia remain a mystery.
What is Microtia?
When a normal ear develops, it includes an external ear fully formed, and a middle ear that carries sound waves to the brain. Patients with microtia do not have a normal external ear. Instead, many come into this world with a small nub or nodule where the ear should exist.
Usually this occurs when the outer ear partially forms during fetal development. Because the internal ear canal becomes blocked, most patients experience difficulty hearing. Some may hear distorted sounds, while others may not hear at all. This is more common among children born with microtia affecting both ears.
There are four distinct grades of microtia, ranging from mild to moderate.
* Grade I microtia results when a child develops an almost normal looking ear that is smaller than normal, but functioning.
* Grade II microtia involves developing a partial external ear, resulting in partial loss of hearing. Patients with grade II microtia may have a closed external ear canal, allowing them to hear only muffled sounds.
* Grade III microtia, the most common form of microtia, involves the lack of an external ear and ear canal, as well as eardrum. Patients with Grade III microtia often have a tiny nub or piece of skin where the external ear should reside.
* Grade IV microtia is the most severe form of the defect, where patients have no ear and accompanying anatomical structures of the ear.
Thanks to modern technology, for patients with partial hearing, and part of the ear or a nub may undergo surgery to produce a normal-looking ear. Typically, children make better candidates for surgery than adults.
How Microtia Affects Children
For most children, having a birth defect as small as results in few problems, until the child reaches the school years. When children are five and older, they start realizing their ear is different from that of their peers.
Many children become the target of cruel taunting or unwelcome stares from other children and even adults that are not familiar with the defect. With time, children with microtia often become self-conscious and may suffer from low self-esteem or other emotional problems.
Despite a parent's best efforts at helping their child feel normal, for most children, it is difficult to live in a world where you "look" different and subsequently "feel" different from your peers.
New Treatments For Microtia
In the past, doctors had few tools available to help children born with microtia. Many doctors recommended patients do nothing, and suggested parents work closely with their child and a psychologist to overcome the stigma associated with a birth defect.
Some patients preferred to cover their deformity in times of old. For many, wearing an artificial ear or prosthesis felt better than showing the world their deformed ear. Unfortunately, prosthetic devices created for the ear can be cumbersome. Most patients must replace them a minimum of twice each year as the child grows. For adults, wearing the prosthesis is less of a problem.
Thanks to modern technology and the work of an innovative plastic surgeon, Dr. Robert Ruder, children can now undergo surgery that essentially creates a new ear.
How To Create The Human Ear
Patients interested in surgery must undergo a several tedious surgeries. Surgery to correct microtia occurs in distinct stages over two years. However, once completed, most patients report they are happy with the results.
Many patients not only look normal, they also hear better because microtia may not affect the inner ear canal. Dr. Ruder created a procedure that allows a new ear to be crafted from grafts of human skin and a tiny piece of the patient's rib.
Sound like a miracle? For many this new surgery is, changing the lives of hundreds of patients suffering from microtia. While expensive, some insurance companies cover part or all the cost of surgery.
Microtia surgery is ideal for young children, but does present complications for adult patients interested in the surgery. While a doctor may rebuild an ear in an older patient, often the result is less aesthetically pleasing as it might be in a child. Regardless, children and adults alike are eager to take advantage of the latest technologies.
Microtia surgery can help children grow up to lead normal, happy and confident lives.
Microtia refers to a condition in which the ear is underdeveloped. Microtia occurs in about one out of every 7,000 to 8,000 births. No one can say for sure why microtia occurs. It usually affects one ear, but may affect both ears. Often microtia is associated with other conditions or syndromes that disfigure the face or head. Even if one or both parents have microtia, the condition is not necessarily passed on to their children.
Like the external ear, the middle ear, which transmits the sounds that are heard, may also be incompletely formed. As a result, hearing in the microtic ear may be markedly distorted or completely absent. As a rule, the degree of hearing impairment is usually associated with the severity of the microtia. It is a good idea to have your child's hearing evaluated and monitored regularly by an otolaryngologist.
Even though your child may not seem to be bothered by the malformed ear, feelings of self-consciousness may potentially develop. The deformity of the outer ear often draws attention from others, especially children. Children generally become very aware and curious of differences in their bodies around the age of 4 or 5. By age 6 or 7, children begin to tease other children who do not look 'normal'. As a result, the child with a microtic ear may not be accepted by other children of the same age. This can produce feelings of self-consciousness and inadequacy.
There are three possible treatment options for the child with microtia. The first option is to do nothing, however, the potential to develop psychological scars remains. The second option is to cover up the deformity. An artificial ear, called prosthesis, can be worn to hide the microtic ear. The ear prosthesis requires replacement about twice a year to keep the size and color matched to the child's growth. The third option is to surgically correct the deficit. Surgical correction is done in a series of stages and can be completed within two years. These options can be discussed with the doctor to help you choose which option is best for your child.
Readmore...
Thursday, January 8, 2009
Surgeries for Lips and Chin
Thick Lips
Thick or fat lips are reduced in size by removing a strip of the red mucosa of the lip along with the underlying tissue from one end to the other end.
This surgery is done under local anesthesia without any hospital stay.Both the lips can be reduced at the same time.This procedure also can be combined with other facial surgeries.
Double Chin
Double chins are corrected by removing the excess of fat under the jaw bone by suctioning method or by open method through a small cut under the jaw bone.
The latter method is preferred if the muscles also have to be tightened. Double chins can be corrected under local anesthesia without any hospital stay.This can also be done along with face lift.
Receded Chin
Patients with a receding chin but with normal dental bite (Dental Occlusion) are good candidates for augmentation of the chin. If there will be an abnormal dental bite, that should be corrected first and then the chin should be revaluated for augmentation.
A cut is usually made inside the mouth just below the gum or under the chin on the outside skin and a silicone implant is placed in front of the chin bone. This surgery is done under local anesthesia and requires no hospital stay.
Readmore...
The Cosmetic Surgery Center of Ohio - Breast Augmentation
Breast augmentation:
Enlargement of the breasts. Augmentation of the breast typically consists of insertion of a silicone bag (prosthesis) under the breast (submammary) or under the breast and chest muscle (subpectoral) and then filling the bag with saline (salt water). This prosthesis expands the breast area to give a fuller breast (increased cup size), give a better contour, and give more cleavage.
The ultimate size of the breast is mainly a personal decision by the patient. Cup size is an inexact estimate of the final size since cup sizes vary with the bra manufacturer and how tight or loose the patient wears her bra as well as how much breast tissue is already present. Describing the preferred cup size does aid the surgeon, but it also helps to look at pictures or photos to show the physician the desired final look.
The most accurate method of estimating the implant size (in ounces) is to fill a plastic bag with measured amounts of water and place in a bra with the patient's estimated cup size. One can see with the bra on and covered by a sweater what the final result will approximate.
Patients most often comment that, "I wish I had gone larger," although there is a rare patient who feels she is too large.
The incision (cut) may be placed at various locations such as: under the breast at the breast fold; periareolar which is at the edge of the areola (brown area consisting of nipple and areola); within the areola; in the armpit (axillary); or in the umbilical area.
The thinnest scar is usually in the areola. The umbilical incision approach is used with an endoscope (tube with a light for visualization and placement of the breast implant).
The smooth surface implant requires a large pocket and is associated with a 10% incidence of capsule contracture (tightening of the scar around the implant causing firmness or hardness). The smooth implant has only an occasional occurrence of rippling or wrinkling which gives the overlying skin a wavy appearance.
A textured (roughened surface) implant is associated with a 3% incidence of capsule contracture but has a 7-9% occurrence of rippling.
What are the choices of implant positions? The easiest surgical placement of the implant is under the breast tissue (submammary).
A slightly more difficult surgical placement is under the chest muscle (submuscular or subpectoral) but this position is associated with a lower incidence of capsule contracture and slightly less occurrence of rippling. There is more pain postoperatively than with a submammary placement.
Readmore...
Eyelid Surgery (Blepharoplasty)
Eyelid surgery (blepharoplasty) is a popular cosmetic plastic surgery to remove excess skin, fat, or muscle from the upper and lower eyelids. Blepharoplasty cosmetic surgery improves baggy skin under the eyes, sinking upper eyelids, or drooping eye lashes that impair vision. The surgery may also be performed to treat a medical condition called ptosis (drooping eyelid), which is caused by poor muscle tone or nerve damage. Ptosis causes the eyelids to hang very low and block vision.
Blepharoplasty treats drooping eyelids, but not drooping eyebrows or wrinkles. Blepharoplasty is often performed with another cosmetic surgery such as abrow-lift or facelift to improve droopy eyebrows, crow's feet, and facial sagging.
Why Blepharoplasty?
As we age, excess skin forms in the eye area and the skin loses elasticity. Fatty tissue can accumulate under the skin. Your eyes will "look older" because these aging processes leave the eyes appearing tired, wrinkled, or puffy. Even with a good skincare and eyecare regimen, wrinkles, puffiness, and drooping eyelids will catch up to you. Genetic factors and body chemistry can cause these aging effects in younger people. Plastic surgery may restore a youthful and refreshed appearance to your eyes.
Is Blepharoplasty Right for Me?
The best candidates for blepharoplasty are physically healthy, emotionally stable, and well-informed about the procedure. Ideal candidates are typically at least 35 (although genetic factors may indicate treatment for younger patients). Candidates may be excluded if they suffer from any of the following conditions: dry eyes, high blood pressure, hypothyroidism, cardiovascular disease, diabetes, glaucoma, or Graves' disease. Personal anatomy issues, including bone and supporting structure, may also affect your candidacy.
The Blepharoplasty Procedure
Incisions are made along the line creases of the upper eyelid and possibly along the outer lower rim of the eye's skin. When removing fatty tissue, but not skin, the surgeon may perform a transconjunctival blepharoplasty with an incision inside the lower rim of the eye's skin. These incisions often reach the outer corners of the eyes. The surgeon then divides the fatty tissue and muscle from the skin so that excess skin, fat, or muscle can be removed.
The blepharoplasty procedure is often performed under local anesthesia — while you are sedated, numbed, and awake — in an outpatient surgery center, surgeon's office, or hospital. General anesthesia (while you are asleep) may be used. Be sure to discuss the appropriate type of anesthesia with your doctor and the anesthesia provider. Depending upon the number of eyelids and extent of the procedure, time in surgery may be up to three hours. Patients return home typically within hours of the surgery.
After Blepharoplasty Surgery
The eyes will often be lubricated and covered with bandages after surgery. Pain and discomfort can be managed with oral medications. Unmanageable pain should be reported to your doctor immediately. The doctor will also prescribe an antibiotic to prevent infection. You will receive a list of instructions to follow for a number of days, including
* the proper way to clean your eyes
* use of cold compresses
* use of lubricating eye drops
* head elevation
* no makeup
* no alcohol
* no television
* no contact lenses
Stitches are removed about a week after surgery. Bruising and swelling will continue to decrease after stitches are removed. Sunglasses and a protective sun block are required for several weeks. Normal activities can be resumed after about ten days. Strenuous activities such as lifting, bending, or exercise can be resumed after about three weeks.
Complications and Risks of Blepharoplasty
Following surgery, patients may experience tearing, itchy, burning eyes, dry eyes, light sensitivity, and blurred or double vision, which can persist for several days. These complications can be relieved with lubricating eye drops. There will also be some swelling around the eyes. Scarring is another possible complication. Sometimes patients will have difficulty closing their eyes when asleep: although very uncommon, this complication can be permanent. The lower lids may appear to be pulled down: this rare condition, called ectropion, may require additional surgery. There also may be some asymmetry to the eyes.
As with any surgery, there is risk of complications related to infection or reaction to anesthesia. You can avoid most complications by selecting the right plastic surgeon and following pre- and postoperative instructions. With proper precautions by the surgical team, complications are typically minimized or prevented. During consultation with a qualified plastic surgeon and ophthalmologist, your medical history and vision will be evaluated to assess candidacy and risks.
Consult a Qualified Surgeon
Before deciding on blepharoplasty, be sure to discuss the options with aboard-certified plastic surgeon and an ophtalmologist. The plastic surgeon and eye surgeon should have extensive experience performing blepharoplasty. Surgeons can show you the photos of other blepharoplasty patients with similar eyelids. You can look at these pictures to help create your individual surgical plan, as well as get a better idea of what to expect from plastic surgery.
Here are some guidelines to consider when consulting a plastic surgeon:
* Ask about credentials, training, and the number of times the treatment has been performed in the practice.
* Discuss the type of anesthesia to be used.
* Find out where surgery will be performed (surgical suite, hospital, other facility).
* Ask about the extent of the eyelid reshaping, and any associated procedures you may be having.
* Ask about the recovery period and limitations on your activities.
* Ask for an explanation of risks, possible complications, and likely results.
Blepharoplasty Costs
Since blepharoplasty may be performed to reduce fatty tissue, skin, and muscle, the extent of the procedure can vary, which makes it difficult to give a range or an average cost. Each eye may have a different cost. The average cost for blepharoplasty is hard to estimate accurately until you are examined by a surgeon and have discussed a surgical plan.
Blepharoplasty plastic surgery comprises three costs: anesthesia fees, facility fees, and surgeon's fees. Since blepharoplasty is often performed during a brow-lift, facelift, or chemical peel, anesthesia and facility fees can be combined with the other procedures. The total fees can range from $2,000 to $5,000 or more, depending on the extent of the procedure.
Some of the cost can be covered by insurance if the blepharoplasty is related to ptosis or other medical necessity. Be sure to ask your surgeon about filing for insurance. Blepharoplasty for purely cosmetic reasons is not covered. If you are having a medically necessary procedure, and want to add on a cosmetic procedure performed at the same time, you can save out-of-pocket cost by combining the necessary and cosmetic procedures into the same facility and anesthesia fees.
Payment
If the cost is more than you can pay at once, ask your surgeon about monthly payments. For financing options and tips, continue reading about Patient Financing.
Readmore...
Rhinoplasty (Nose Job) at www.PearsonFaces.com
What Is a Rhinoplasty and Why Is It Done?
Rhinoplasty ("nose job") is the surgical alteration of the nose to change its shape or improve its function. Rhinoplasty is performed to correct breathing problems related to the nose or to correct disfigurement of the nose that has occurred because of trauma or birth defects that cause the nose to take an abnormal shape. Cosmetic rhinoplasty is performed on normal noses to improve their shape and appearance. Rhinoplasty can reduce or increase the size of your nose, or change the size or shape of the tip, the bridge, or nostrils.
Who Is a Good Candidate For a Cosmetic Nose Job?
A good candidate for a cosmetic nose job is anyone who is unhappy with the appearance of his or her nose and is looking for an improvement in the way he or she looks. Candidates should also be in good physical health, be psychologically stable and have realistic expectations.
How Do I Know If My Expectations Are Realistic?
If you are considering rhinoplasty, be sure to discuss your expectations with your surgeon. During your initial consultation, you will be asked what bothers you about your nose and how you would like to change it.
Also, the surgeon will evaluate the structures of your nose such as the underlying nasal bones and cartilage, your overlying skin and your other facial features. After this evaluation, the surgeon can tell you if expectations are realistic and whether the rhinoplasty will enhance your natural facial beauty.
Is There a "Perfect" or "Ideal" Nose?
There is no one nasal shape that will compliment the natural beauty of every face. Today, surgical changes are made to enhance the remaining facial features and emphasize the individual's unique and natural facial beauty. A plastic surgeon can describe the facial features that make you unique and describe the changes that would enhance your appearance.
How Is a Rhinoplasty Done?
Rhinoplasty is usually done as an outpatient procedure under either general or local anesthesia. With general anesthesia, you sleep through the operation. With local anesthesia, you are sedated and the nose is numbed so you are relaxed and unable to feel the pain. The incisions are made within the nostrils and in more difficult cases may also be made across the base of the nose. The inner bone and cartilage are reshaped to produce a more pleasing shape.
What Is a Structure Rhinoplasty?
A structure rhinoplasty is a technique where only minor amounts of cartilage are removed. The change in shape is obtained by remolding the existing cartilage or by adding cartilage grafts. Because only a small amount of cartilage is removed, the structural strength of the nose is maintained and this ensures that the shape will not change over time as the nose heals.
How Long Does It Take To Recover From a Rhinoplasty?
A nasal splint is normally worn for the first week after rhinoplasty. You can expect swelling and some bruising around the eyes after surgery which will begin to improve after the third day, but lasts up to two weeks.
After that, you will have a minor degree of swelling noticed only by you and your surgeon. This swelling will go away over the next six months. The final shape of your nose will be apparent after it has healed completely.
You should avoid strenuous activity for three to four weeks after surgery. You may return to your social activities in as soon as two to three weeks without any recognizable appearance that you had surgery.
Will Insurance Cover a Rhinoplasty?
It's important to realize that elective, cosmetic surgery is not typically covered under most insurance plans. Most insurance companies, however, typically cover that which is medically necessary. Coverage will depend on your insurance carrier.
Readmore...
Hair Transplantation
Introduction
Providing the reader with all of the tools necessary to select patients properly, design a treatment plan, and perform hair transplantation would be impossible within a single article. The purpose of this article is to provide a broad overview of the techniques used by many hair transplant surgeons, which serves as a foundation for the hair transplant surgeon. Hair transplantation is as much an art as it is a science, requiring both technical skill and artistic creativity.
Patient Selection and Preoperative Preparation
Hair transplantation is a surgical modality used for the correction of androgenic alopecia, scarring alopecia, and other causes of permanent alopecia. Since hair transplantation is a surgical procedure, all patients must be in good health. Many surgeons perform preoperative laboratory studies that include complete blood count, platelet count, serum chemistries, prothrombin time, pre–prothrombin time, and bleeding time. Some surgeons also check for human immunodeficiency antibodies, hepatitis B surface antibodies, and hepatitis C antibodies.
As with any cosmetic surgical procedure, the patient must have reasonable expectations. In fact, dissatisfaction after hair transplantation often arises from changed or unreasonable expectations rather than from complications or poor results. During initial consultation, the physician must learn the patient's goals and the circumstances that brought the patient to the decision to consider hair transplantation.
In addition, the physician must examine the patient, recognize the underlying cause of the patient's hair loss, and estimate the effect that time will have on the hair loss process. The patient must be provided with ample time to ask questions and arrive at a complete understanding of the procedure, expected outcome, and the changes that can be expected over time (eg, how results will change with future hair loss). Together with the patient, create a logical plan that will impart a natural-looking result both now and in the future.
Provide patients with both written and oral preoperative instructions. They need to be instructed to discontinue blood-thinning agents well before surgery to normalize bleeding time. Most surgeons require patients to discontinue aspirin or aspirin-containing products a minimum of 7-10 days before surgery. Nonsteroidal anti-inflammatory medications (eg, Advil, Motrin, Aleve) must be discontinued depending on the half-life of the agent. Consumption of alcoholic beverages has been shown to increase bleeding tendency and should be stopped a minimum of 7 days before surgery. Excessive vitamin E consumption is believed to increase bleeding tendency, and most surgeons advise patients to discontinue vitamin E supplements a minimum of 1 week before surgery. Consider inquiring about dietary and nonprescription alternative medications, since the list of herbal supplements that affect bleeding is growing.
Preoperative Skin Preparation
To reduce risk of intraoperative wound contamination, many surgeons require patients to shampoo with 4% chlorhexidine gluconate the night before surgery. Note that significant keratitis has resulted from chlorhexidine remaining in the eye during surgery; therefore, one must instruct all patients to keep the cleanser out of their eyes. In addition, rare reports of anaphylaxis have been reported. Alternatives to chlorhexidine include Betadine shampoo, 3% chloroxylenol (Techni-Care), Dial liquid antimicrobial soap, and pHisoHex. In addition, some surgeons also require patients to shampoo their hair the morning before surgery and abstain from using hair products (eg, gel, mousse, hair spray).
Surgical preparation
Both the recipient and donor sites are scrubbed with 4% chlorhexidine gluconate or povidone-iodine (Betadine) solution. Some surgeons prefer to place the patient in a prone position when harvesting follicular grafts, while others seat patients for both harvesting and placing grafts. Hair at the donor site most often is trimmed to 1-mm length using scissors or an electric trimmer. To provide better exposure of the donor site, some surgeons prefer to tape the hair superior to (above) the donor site or to use sterile Kling gauze to improve visualization.
Anesthesia
In addition to local anesthesia, some surgeons also administer sedatives prior to and during the procedure.
Methods of administration
Most surgeons administer local anesthesia using a traditional syringe and a 30- or 27- gauge needle. A novel device has been created that precisely controls the infusion rate and pressure of local anesthetic using a microprocessor pump. This device, called the Wand or CompuMed - Featuring the Wand Handpiece, has been shown to produce less pain and discomfort than traditional injection.1
Donor site
Several methods are used to provide anesthesia to the donor site. Some surgeons prefer to infiltrate the donor site locally or use a ring block using 1% or 2% lidocaine with 1:100,000 epinephrine. Other options include using a mixture of 1% lidocaine with 1:100,000 epinephrine and 0.5% bupivacaine or 0.5% lidocaine with 1:200,000 epinephrine.
Regardless of which concentration and agents are used, good skin turgor aids the surgeon when harvesting donor tissue and is extremely important when using punch harvesting or multistrip harvesting techniques. Consider the total dose of lidocaine, and ensure that nontoxic doses are used.
Recipient site
Local infiltration after completing a ring block remains the most commonly used technique for achieving anesthesia of the recipient site. Many surgeons use 1% lidocaine with 1:100,000 epinephrine, 2% lidocaine with 1:100,000 epinephrine, 0.5% lidocaine with 1:200,000 epinephrine, or a mixture of lidocaine with epinephrine and bupivacaine.
Tumescent anesthesia using standard Klein solution has been used and provides good anesthesia. Regardless of which method of anesthesia is used, ensure that the total dose of lidocaine remains below the toxic level.
Procedure
Donor harvesting
A number of different techniques are available for harvesting hair follicles; each technique has advantages and disadvantages. Regardless of which harvesting technique is used, the principle of protected hair follicles remains paramount. It is well known that some hairs are not lost to androgenic alopecia. Usually, the protected follicles are found in the inferoposterior scalp and inferior parietal scalp. It is essential that only protected follicles be transplanted to ensure maximal survivability. With any of the below techniques, the punch, blade, and blades used are angled parallel to the hair follicles and not perpendicular to the scalp itself in order to minimize transection of hair follicles.
Punch harvesting
This technique was used most commonly for harvesting donor follicles until the late 1980s or early 1990s, when excision with or without a multibladed knife became used more widely because of its many advantages. With the punch harvesting technique, a small hand engine is used (which spins approximately 10,000-15,000 revolutions per minute) with a 2- to 6-mm punch. As the punch spins, it is pressed into the donor scalp parallel to the hair to minimize transection of any hair follicles. When the desired depth is achieved, the punch is withdrawn and moved to the next donor site to be excised.
Once punching of the number of grafts desired is complete, the graft may be lifted gently, using forceps or a sterile needle, and cut free using scissors (leaving approximately 1 mm of fat at the base of follicle). Defects created from harvesting may be left to heal by secondary intention or may be closed using sutures or skin staples. Healing by secondary intention has been abandoned, largely because of results that are cosmetically inferior.
Excision
The donor site is excised as an elongated fusiform ellipse of full-thickness scalp using a scalpel blade size 10 or 15. Take care when excising not to damage hair follicles at the edge of the donor tissue. The resultant defect is closed using suture or skin staples, and the scar is minimal. Then, donor tissue is dissected carefully into the desired number of grafts, which can vary in size.
Strip harvesting
A scalpel containing 2 or more size 15 blades mounted in parallel is used to cut strips of donor tissue. This facilitates the division of donor scalp into minigrafts and micrografts. Several multibladed scalpel handles currently are available that can accommodate as many as 6 or more No. 15 blades, which most commonly are spaced 1.5-2.5 mm apart. This technique may carry a higher risk of follicle transection than excision.
Creating and dissecting grafts
Grafts obtained by punch grafting can be transplanted directly or cut into smaller grafts using a size 15 blade or razor blade. These round grafts can be cut into halves or quarters, or they can be dissected down to single hair grafts. Grafts harvested by excision or strip harvesting can be cut to single grafts, minigrafts, or micrografts by using a size 15 blade or razor blade.
Most surgeons use magnifying loupes or a dissecting microscope to aid the dissection of grafts. Some surgeons believe that follicular grafts (ie, those that are essentially a single follicular unit) offer better results, although further studies are needed.2
Creating recipient sites
Several techniques are used for creating and preparing recipient sites (where grafts are to be placed); each has several advantages and disadvantages.
* Single hair and slit grafting: Using a scalpel with a No. 15 blade or number 3764 beaver blade or an 18-gauge needle, 18-gauge Yeh needle, or NoKor needle, multiple 0.5- to 3-mm slits are made in the scalp in which the grafts are placed (see Dilator use, below) Single hair or micrografting is most often used to recreate the frontal hairline. Magnification with illumination with polarized light emission diodes may reduce the risk of follicle transection during the creation of slits.3
* Dilation (modified slit grafting): Sharp 0.8- to 1.6-mm dilators are inserted directly into the scalp, pushing the scalp aside to provide hemostasis. Micrografting (grafts containing 1-2 hair follicles) or minigrafting can be performed using dilation. Micrografting most often is used to recreate the frontal hairline. This method has not become popular as it is typically slower than slit grafting and may result in compression of the grafts, especially when more than one hair follicle is grafted.
* Punch grafting: Using 1- to 4-mm diameter punches, a defect is created at the recipient site into which the graft may be inserted. Occasionally, bleeding occurs that can be tamponaded easily by inserting a dilator or the graft. The larger the size of the graft, the more likely it is to have what is termed a "doll's hair" or "cornrow" appearance.
* Laser-assisted grafting: Carbon dioxide laser has been used to create recipient sites.4 To date, optimal laser parameters have not been determined. Many surgeons use 35-50 W at an interval of 0.05 seconds. Significant delay in the growth of the transplanted hairs usually occurs after laser-assisted transplantation.
Dilator use
After creating recipient sites, dilators may be used to enlarge the opening, by pushing adjacent scalp aside, and/or to provide hemostasis. In addition, many surgeons believe that this aids in the insertion of grafts; therefore, lesser trauma results to the grafts during insertion.
Graft insertion
Most surgeons use jeweler's forceps or similar small non – toothed forceps to insert grafts. Gently insert a graft by grasping the fat immediately beneath it to minimize trauma to the follicle. Some surgeons use a needle to insert and tease grafts gently into place. More recently, implantation devices have been designed that create recipient site and insert grafts.5
Medications and Postoperative Dressings
Medications
Antibiotic use
Significant controversy remains regarding the use of prophylactic antibiotics in hair transplant surgery, since few studies support the use of antibiotics. Although prophylactic antibiotics can decrease the risk of wound infection, the risk of hypersensitivity reactions and the emergence of resistant organisms need to be considered. The most appropriate time to administer prophylactic oral antibiotics (as single dose) is 1 hour preoperatively; however, if endocarditis prophylaxis is necessary, an additional postoperative dose is administered.
For most patients, first-generation cephalosporin is used, unless a history of cephalosporin allergy exists. If cephalosporin hypersensitivity exists, azithromycin or ciprofloxacin may be substituted. Some surgeons also use topical antibiotics during the postoperative period to reduce risk of wound infection, although no benefit has been established yet. Some surgeons use oral antibiotics for 3-5 days postoperatively to reduce risk of infection.
Corticosteroids
Many surgeons administer oral or intramuscular corticosteroids to reduce postoperative swelling, although few data are available supporting this practice.
Pain medications
Some patients require oral narcotics for the first few days after hair transplantation. Usually, Tylenol with codeine # 3, Percocet, or Lortab 5 is sufficient to alleviate most postoperative discomfort.
Postoperative dressings
Most surgeons advocate use of surgical dressings to minimize risk of graft loss. Many surgeons apply (1) topical antibiotic, (2) Telfa nonstick gauze, (3) gauze, (4) Kerlix gauze, and (5) Coban wrap to create a turbanlike dressing. Most often, this dressing is removed after 24 hours; no dressing is required thereafter. Some surgeons use no postoperative dressing and require patients to wear a baseball cap.
Complications
As with any surgical procedure, a risk exists of the following infrequent complications:
* Bleeding
* Infection
* Scarring at donor site
* Scarring at recipient sites
* Dyspigmentation at recipient sites
* Cobblestone appearance at recipient sites
* Failure of graft
* Cyst formation
Postoperative edema is expected; therefore, it is not a complication, although it can be severe.
Summary
In conclusion, hair transplantation is a surgical procedure used predominantly for correction of androgenic alopecia. Protected hair follicles are transplanted to affected areas using a variety of techniques; each technique has advantages and disadvantages. Significant advances in hair transplantation have made this procedure more popular and have led to superior results, which often are undetectable to the layperson.
Readmore...
Wednesday, January 7, 2009
Tenisson-Randall Cutting
The triangular flap is but one of several methods of creating a flap in an otherwise straight line closure of the lip closure may be high or low and various surgeons promote their specific choice of location.
Although the rotation advancement technique of Millard has the greatest number of followers and is recognized as a simple method once experience is obtained, a number of surgeons prever a triangular technique, since it seems simpler to lay out and perform and is less of a “cut as you go” free hand performance. For some surgeons it seems simpler and easier to teach and possibly more reliable for those performing and teaching a small number of cases.
The Tennison triangular flap technique described by Randall demonstrates that the medial lip element contains the essential landmarks for Cupid’s bow. The triangular flap technique recognizes that Cupid’s bow is high on the cleft side. The technique plans for a diagonal incision directly above the raised lateral peak into the philtrum. When the lip element is lowered, a triangular defect is created by incision, which is filled upon closure with the triangular flap from the cleft side. Thus tissue is added to the noncleft side of the lip in the lower one third. This is in contrast to the Millard rotation advancement technique, which advance a triangle of tissue in the upper one third. A distinct difference is that the philtrum is not cut across by the Millard rotation incision. The triangular flap is in the lower one third of the lip and contains full thickness of the lip consisting of skin, muscle, and mucosa.
Advantages of the triangular flap are that it adds length to the medial lip element, rebuilds a good floor of the nostril, preserves Cupid’s bow, and adds tissue in the lower one third of the lip, where it is needed most. Furthermore, it gives dependable results.
The disadvantages are that the Z in the lip crosses the philtral line. It is a confusing technique to explain, especially the height adjustment and placement of the triangle in the lateral lip element. Furthermore, the vermilion countour is deficient in the midline and there is a tendency to get an increase in lip height on the repaired side. It is not clear how long to construct the lateral lip element, thus increasing the discrepancy in lip length.
Liposuction
Definition of Liposuction
Liposuction: The most common cosmetic operation in the U. S. with over 400,000 such surgical operations done annually, liposuction involves the surgical suctioning of fat deposits from specific parts of the body, the most common being the abdomen (the "tummy"), buttocks ("behind"), hips, thighs and knees, chin, upper arms, back, and calves.
Liposuction breaks up and "sucks" fat out of the body. This is done through a canula (a hollow instrument) inserted subdermally (under the skin). A strong (high-pressure) vacuum is applied to the cannula.
In ultrasonic-assisted liposuction (UAL), the cannula is energized with ultrasonic energy, causing the fat to melt away on contact, an advantage in areas of scar tissue such as the male breast, back, and in areas of prior liposuction. The disadvantages of UAL include the need for longer incisions in the skin, potential for skin or internal burns, greater cost, and longer time.
The technique of tumescent liposuction has become especially popular, in part because of its purported safety. It involves pumping several quarts/liters of a solution below the skin (subcutaneously) in the area to be suctioned. The solution is salt water (saline) to which is added the local anesthetic lidocaine to numb the area and the vessel-constrictor epinephrine (adrenaline) to help minimize bleeding. The fat is suctioned out through microcannulas (small suction tubes). Tumescent liposuction is now the most used form of liposuction.
Five deaths after tumescent liposuction were found among 48,527 deaths referred to the Office of Chief Medical Examiner of the City of New York from 1993 to 1998, according to a report published in The New England Journal of Medicine.
The 5 victims ranged from 33 to 54. Four of the 5 were women. All 5 had received lidocaine. Three died because their heart rate became too slow (bradycardia) and their blood pressure dropped precipitously (hypotension). It is well known that lidocaine lowers the heart rate. In fact, it is sometimes used as an emergency measure to slow dangerously rapid heart rates.
One patient died of fluid overload. She had been given more than 13 quarts of fluid, 7 intravenously and 6 pumped into the surgical sites which included the breasts (for enlargement), chest, arms, back, abdomen, thighs, buttocks and knees. The excess fluid collected in her lungs (pulmonary edema) and she essentially drowned to death.
The fifth patient died of a blood clot in the lungs. She had tumescent liposuction of the legs, developed thrombosis (clot) in her calf veins, the clot broke loose (embolized) and wedged in her lungs (pulmonary thromboembolism).
Tumescent liposuction can be fatal, conclude the authors of the report, Drs Rama B. Rao and Robert S. Hoffman of New York University Medical Center and Bellevue Hospital and Dr. Susan F. Ely, forensic pathologist in the Office of the Chief Medical Examiner of New York City. The danger of tumescent liposuction appears to be due, at least in part, to the lidocaine -- the toxicity of lidocaine and untoward interactions of lidocaine with other medications the patient may be taking.
No matter how liposuction is done, it is considered completely cosmetic and therefore completely elective (entirely optional). The central question now looming with liposuction would seem to be: "Are any deaths justifiable with a completely cosmetic procedure?"
Readmore...